
Proposed Hypoxic "O2" Pipeline Algorithm
Copyright 2002 University of Florida Department of Anesthesiology
Version 1.1
May 13, 2002
Disclaimer
The discussion and proposed algorithm below are based on anesthesia
machine designs used in the United States and may not be appropriate
for designs that adhere to different regional or national standards
and practices.
Diagnosis
Fault 2 on the Virtual Anesthesia Machine (www.anest.ufl.edu/vam) is
a hypoxic O2 pipeline condition (gas mix-up) where N2O, instead of O2,
is inadvertently supplied to the O2 pipeline. This fault recently occurred
in New Haven, CT in January 2002 and contributed to the death of 2 patients.
Even though an anesthesia machine was not involved in the New Haven
cases, the root cause is applicable and clinically relevant to anesthesia
machines.
Observations/Consequences
1. N2O is supplied, instead of O2, via the O2 flow meter
2. N2O is supplied, instead of O2, when pressing the "O2 flush"
valve
3. The "O2 failsafe" device is fooled and allows delivery
of a hypoxic gas mixture
4. The "hypoxic guard" device (O2 proportioning device) does
not prevent delivery of a hypoxic gas mixture
5. N2O is used as the drive gas, instead of O2, during mechanical ventilation
6. N2O, that is now the drive gas, is vented directly to the room in
most anesthesia ventilators with gas driven bellows
7. The O2 analyzer, if present, alarms when FiO2 drops below alarm threshold
8. The pulse oximeter, if present, alarms when SpO2 drops below alarm
threshold
9. Initially, end-tidal CO2 will be normal if ventilation (not oxygenation)
is adequate
10. Airway pressure will be normal if ventilation is adequate
Rationale and discussion of the observations and consequences
Recommended Algorithm
If a hypoxic O2 pipeline condition is suspected because of a
low FiO2 alarm and/or reading that does not match the set FiO2:
Note that this implies that an O2 analyzer is being used
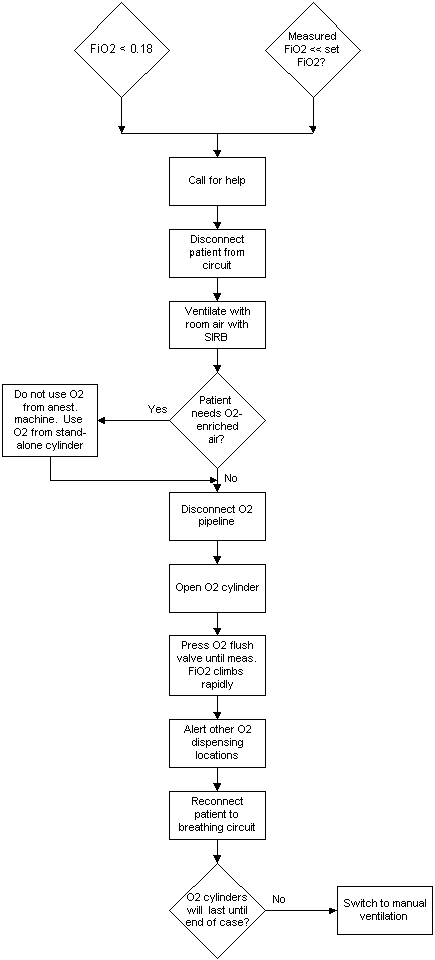
(a) Call for help (for example, anesthesia technicians, other clinicians,
911)
(b) Disconnect the patient from the circuit at the elbow connector with the gas sampling line still attached to the elbow connector
(c) Ventilate (or ask for assistance to manually ventilate) with a
self-inflating resuscitation bag (SIRB or "Ambu" bag) using
room air. If the patient needs O2-enriched air, use O2 from a stand-alone
O2 cylinder.
(d) Disconnect O2 pipeline - in most machines, an audible alarm should
sound confirming O2 pipeline disconnection if the machine is turned
on
(e) Open the O2 cylinder - in most machines, a sound or cessation of the audible alarm in (d) should indicate that O2 cylinder is open and not empty
(f) To clear the anesthesia machine of the hypoxic gas, press the oxygen
flush button until the O2 analyzer displays increasing FiO2 values
(g) Alert all other locations supplied by the same central oxygen supply
(h) Reconnect breathing circuit to patient, resume ventilation (mechanical or spontaneous) using O2 from the O2 cylinder on the anesthesia machine and order more O2 tanks
(i) If extra O2 cylinders are not readily available and an O2-driven
mechanical ventilator (which consumes a lot of O2) was previously being
used, switch to manual ventilation to conserve the O2 used as ventilator
drive gas and extend the time to exhaustion of the O2 cylinder.
Rationale and discussion for proposed
algorithm above when oxygen analyzer is available.
Recommended Algorithm if an O2 Analyzer is Not
Being Used
If an O2 analyzer is not being used, there will be no low FiO2 warning.
The first indication of trouble will most likely be a low SpO2 alarm
that is a late and non-specific warning. Because of the non-specificity
of a low SpO2 alarm, there are many possible causes to be ruled out
before a hypoxic O2 pipeline algorithm as outlined above can be initiated
with certainty.