
To reference this electronic educational resource according to the APA style for Web references, use:
Liem EB (2006): Lighted Stylet Intubation. Retrieved <insert date of retrieval here>, from University of Florida Department of Anesthesiology, Center for Simulation, Advanced Learning and Technology, Virtual Anesthesia Machine Web site: http://vam.anest.ufl.edu/airwaydevice/lightedstylet/index.html
Keywords: Lighted stylet, lightwand, Intubation, difficult
airway, airway management
Also known as Trachlite (Rusch), Trachlight (Laerdal), Surch-lite (Aaron Medical), "Lightwand"
See videos in the video library
Introduction
Lighted stylet guided intubation can be a useful technique for oral and nasal intubations in both asleep and awake patients (1,3). This type of intubation technique has a reported success rate as high as 99% in experienced hands (3). It can be used in anticipated and unexpected difficult airways where conventional direct laryngoscopy has failed (2,7). It can be achieved as fast as conventional direct laryngoscopy by one skilled in its use (3,4,5). Sufficient skill is obtained after approximately 15 intubations with the lighted stylet. Manipulation of the head and neck can be kept minimal and the patient does not require a wide mouth opening (6-8 mm) which makes this technique extremely useful in certain subpopulations of patients. This technique may also be helpful in patients with anterior larynx, scarring, or a bloody airway, because the lighted stylet has no optical viewing element. A decreased incidence and severity of sore throat, hoarseness and dysphagia has also been reported in comparison to direct laryngoscopy (6).
However, because it requires translumination of the soft tissues in the neck, this type of intubation may be less suited for environments in which there is too much ambient light. In a dark environment, a lighted stylet that is correctly positioned in the glottic opening, will show a bright red, teardrop shaped glow in the anterior neck. This glow will be visible at the thyroid cartilage or distal to it. In patients who have a thick or short neck, or are darkly pigmented, identification of this glow can be more difficult. In the thin patient the opposite may occur, where an incorrectly positioned lighted stylet (in the esophagus) still seemingly produces a typical pre-tracheal glow (false-positive). Since there is no direct visualization of the laryngeal structures, this technique should be avoided in patients with known anatomical abnormalities of the upper airway (tumors, polyps, infection, foreign body, upper airway trauma) (1). A recent review of lighted stylet intubations is in consistent agreement with our experience and recommendations (8). Because of the lightbulb size, the particular lighted stylet discussed here cannot be used in the pediatric population that requires endotracheal tubes smaller than 5.5 ID.
Preparation
One type of lighted stylet currently being used is the Surch-lite®.

- Select Endotracheal Tube (ETT): smallest possible size for use with the lighted stylet is 5.5 mm inner diameter.
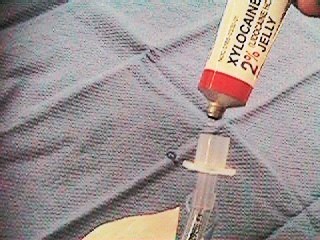
- Apply a water-based lubricant to ETT opening (e.g. Lidocaine jelly, K-Y jelly, Hurricaine spray). Lubrication is essential to advance the ETT without it sticking to the stylet.
- Test lightsource. If the light does not work, the batteries can be replaced by depressing and twisting the cap switch 90 degrees (although this is unlikely as these devices are disposable)
- Insert lighted stylet until the lightsource reaches the tip of the ETT. When the stylet is in the correct position, engage the locking piece into the ETT connector and secure.
- Bend the ETT/lighted stylet assembly to a sharp angle of slightly GREATER than 90 degrees. (This is why prior lubrication of the ETT is an essential step. The sharp angle is necessary if the patient is going to be intubated with the head in a neutral position.) Two different approaches are taken in determining the location of the bend of the ETT/lighted stylet assembly. Some people feel the success rate of the intubation is higher if the bend is placed at the same distance as the distance from the patient's thyroid cartilage to the angle of their mandible. This will essentially measure the distance from the posterior pharynx to the glottic opening. Others prefer placing the bend at a relatively shorter distance (just proximal to the cuff) in order to avoid placing the lighted stylet too posterior and directly into the esophagus. This also makes maneuverability easier if you are rotating a smaller "arm" across the soft tissues during attempts to position the tip at the glottic opening.
Preparation StepsApply
lubricant |
 |
Oral Intubation: A Step by Step Guide
- Induce patient as if for regular intubation; apply cricoid pressure if Rapid Sequence Intubation is desired.
- Darken the OR (this may include extinguishing overhead, OR, and X-ray viewbox lights plus covering the windows).
- Position yourself as for regular direct laryngoscopy. Some people prefer a different approach and like to stand at the side of the patient near the shoulders so that the pre-tracheal glow can be seen more easily, but that does require extra help for masking the patient.
- With the patient's head in neutral position, the non-dominant hand (left for most people) should lift the jaw forward. This will elevate the tongue and epiglottis. This is an essential step as this generates the space in the pharynx through which the ETT/lighted stylet assembly must be navigated.
- Hold the ETT/stylet assembly in the dominant hand and insert it into the mouth.
- If possible, the lighted stylet should be introduced in midline and advanced over the base of the tongue. However, this is often not possible due to the sharp angle of the bend in the ETT/stylet assembly. Alternatively, the lighted stylet can be turned 90 while staying midline, then advanced more deeply via the right or left mouth corner so that it can be brought over the base of the tongue.
- Advance the lighted stylet over the base of the tongue until the pre-tracheal glow is identified. A red downwards streaking glow should be seen (jack-o-lantern effect). The brightness of the glow that should be seen in a particular patient can be gauged before intubation by shining the light through the patient's cheeks. Identification of the typical pre-tracheal glow is the most crucial part of the lighted stylet intubation. A dimmer glow, which is more localized and/or off to the side, indicates a submental or piriform fossae location. In that case, withdraw the ETT/stylet assembly slightly and re-advance. Obtaining the correct glow may require quite a few number of repositionings and may not be achieved on the first attempt.
- Move non-dominant hand from the mandible to the lighted stylet handle and advance the ETT which is still being held with the dominant hand to the desired depth. While advancing the ETT, the pre-tracheal glow can often be observed to travel with the ETT tip down the neck, as the ETT acts as a light pipe.
- Remove lighted stylet, confirm ETT position, inflate cuff and proceed as for regular intubation.
- When withdrawing the lightwand, confirm that the lightbulb is still present.
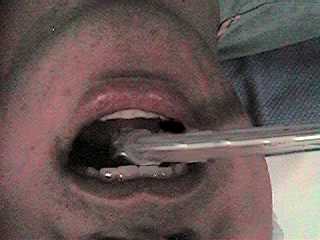
Intubation Steps Insert
via right mouth corner |
 |
Troubleshooting Tips
Cannot find pre-tracheal glow
Not enough space to maneuver:
Increase mandibular distraction and/or instruct someone to use gauze to pull on the tongue.Lighted stylet is stuck in a piriform fossae or in the vallecula:
Advance the lighted stylet over the posterior pharynx instead of tongue base.Patient too obese - cannot see glow:
Have an assistant spread the skin of the neck laterally. This will decrease the distance from the throid cartilage to the skin.
Difficulty advancing the ETT
Stylet may be stuck in the vallecula, giving impression of a pre-tracheal glow:
Withdraw and re-advance more posteriorly.The ETT is getting stuck on the vocal cords:
Withdraw and re-advance, change to smaller diameter ETT if necessary.
Webauthor: E.B. Liem
Consultants: D. Gravenstein
Contributors: J. Payabyab, M.E. Mahla
- Hung-OR, Stewart-RD. Lightwand intubation: I A new lightwand device. Can-J-Anaesth. 1995 Sep; 42(9): 820-25.
- Hung-OR, Pytka-S, Morris-I, Murphy-M, Stewart-RD Lightwand intubation: II Clinical trial of a new lightwand for tracheal intubation in patient with difficult airways. Can-J-Anaesth. 1995 Sep; 42(9): 826-30.
- Hung-OR, Pytka-S, Morris-I, Murphy-M, Launcelott-G, Stevens-S, MacKay-W, Stewart-RD. Clinical trial of a new lightwand device (Trachlight) to intubate the trachea. Anesthesiology. 1995 Sep; 83(3): 509-14.
- Ellis-DG; Stewart-RD; Kaplan-RM; Jakymec-A; Freeman-JA; Bleyaert-A. Success rates of blind orotracheal intubation using a transillumination technique with a lighted stylet. Ann-Emerg-Med. 1986 Feb; 15(2): 138-42.
- Ellis-DG; Jakymec-A; Kaplan-RM; Stewart-RD; Freeman-JA; Bleyaert-A; Berkebile-PE. Guided orotracheal intubation in the operating room using a lighted stylet: a comparison with direct laryngoscopic technique. Anesthesiology. 1986 Jun; 64(6): 823-6.
- Friedman-PG; Rosenberg-MK; Lebenbom-Mansour-M. A comparison of light wand and suspension laryngoscopic intubation techniques in outpatients. Anesth-Analg. 1997 Sep; 85(3): 578-82.
- Holzman-RS; Nargozian-CD; Florence-FB. Lightwand intubation in children with abnormal upper airways. Anesthesiology. 1988 Nov; 69(5): 784-7.
- Davis-L; Cook-Sather-SD; Schreiner-MS. Lighted Stylet Tracheal Intubation: A Review. Anesth Analg 2000; 90:745-756.